A foot rash is one of the most common skin problems people deal with. It can show up as redness, itching, peeling, bumps, blisters, or cracked skin. Sometimes it’s mild and goes away quickly. Other times, it can be painful, persistent, or a sign of infection.
If your feet are itchy, burning, or covered in dry patches, this guide will help you understand what’s happening and how to fix it. We’ll break down causes, symptoms, treatments, prevention tips, and when to see a doctor all in clear, practical steps.
What Is a Foot Rash?
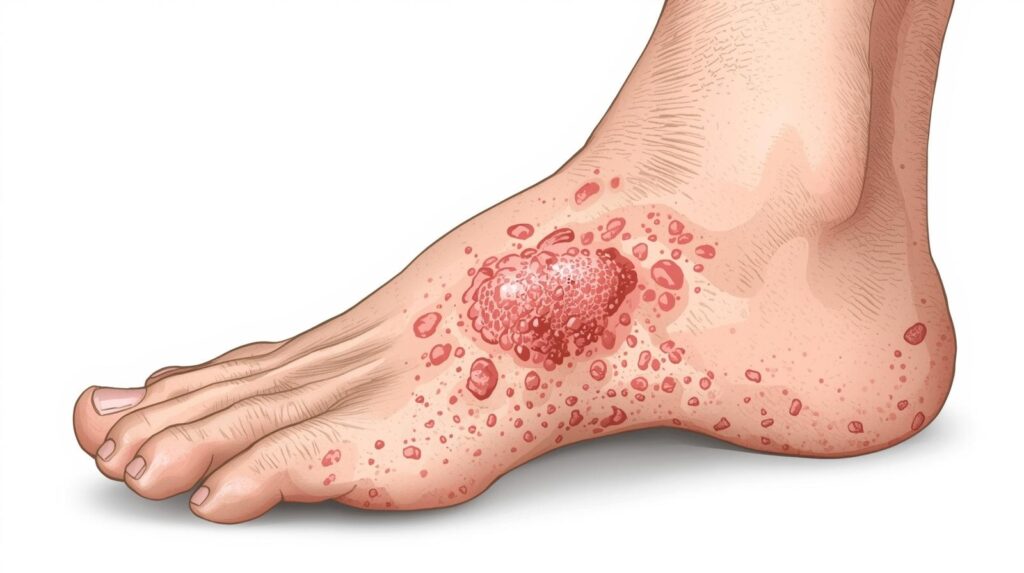
A foot rash is an area of irritated or inflamed skin on the foot. It can affect the top of the foot, sole, heel, toes, or the spaces between toes. Rashes may be caused by fungal infections, allergies, bacteria, heat, sweat, or skin conditions like eczema.
In simple terms:
A foot rash happens when your skin reacts to irritation, infection, or inflammation.
Common Symptoms of a Foot Rash
The symptoms depend on the cause, but most foot rashes include:
- Red or pink patches
- Itching (sometimes intense)
- Burning sensation
- Peeling or flaky skin
- Cracks, especially on heels
- Small blisters
- Swelling
- Pain when walking
- Thickened or scaly skin
- Oozing or crusting (in severe cases)
What does a foot rash look like?
A foot rash usually appears as red, itchy, or peeling skin on the toes, sole, or top of the foot. It may include blisters, cracks, scaling, or small bumps depending on the cause.
Why Does a Foot Rash Happen?
Your feet are warm, often sweaty, and usually covered by socks and shoes. This creates the perfect environment for irritation and infection.
Common triggers include:
- Excess moisture and sweat
- Tight or non-breathable shoes
- Fungal growth
- Allergic reactions
- Skin sensitivity
- Poor hygiene
- Walking barefoot in public areas
Now let’s break down the specific causes.
Main Causes of Foot Rash
1. Athlete’s Foot (Fungal Infection)
Athlete’s foot (tinea pedis) is one of the most common causes of foot rash.
Symptoms:
- Itchy, burning skin between toes
- Peeling and cracked skin
- White, soggy skin between toes
- Blisters in severe cases
Why it happens:
Fungus grows in warm, moist places like sweaty shoes, gym floors, and locker rooms.
2. Contact Dermatitis (Allergic Reaction)
This happens when your skin reacts to something it touches.
Triggers:
- New shoes
- Rubber or synthetic materials
- Detergents
- Soap
- Fragrances
- Foot sprays
Symptoms:
- Red rash
- Itching
- Small bumps
- Swelling
3. Eczema (Atopic Dermatitis)
Eczema can affect the feet, especially in people with sensitive skin.
Signs:
- Dry, scaly patches
- Severe itching
- Thickened skin
- Cracks that may bleed
Stress, climate changes, and harsh products can trigger flare-ups.
4. Dyshidrotic Eczema
This type causes small, deep blisters on the sides of toes or soles.
Symptoms:
- Itchy fluid-filled blisters
- Peeling after blisters dry
- Painful cracks
Often linked to stress, allergies, or sweaty feet.
5. Psoriasis
A chronic autoimmune condition that may affect the feet.
Signs:
- Thick, scaly plaques
- Silvery-white patches
- Cracked heels
- Nail changes
Psoriasis rashes are usually well-defined and long-lasting.
6. Heat Rash
Heat rash happens when sweat gets trapped under the skin.
Symptoms:
- Small red bumps
- Itching or prickly feeling
- Appears during hot weather
Common in people who wear tight shoes for long hours.
7. Bacterial Infection
If cracked skin becomes infected, bacteria can enter.
Warning signs:
- Swelling
- Warmth
- Pus
- Fever
- Increasing pain
This needs medical attention quickly.
Risk Factors
You’re more likely to develop a foot rash if you:
- Sweat heavily
- Wear tight shoes daily
- Use public showers or swimming pools
- Have diabetes
- Have a weak immune system
- Have a history of eczema or psoriasis
- Don’t dry your feet properly
How to Treat a Foot Rash
Treatment depends on the cause. Let’s break it down clearly.
Step 1: Identify the Cause
Before applying random creams, check:
- Is it itchy between toes? (likely fungal)
- Did it start after new shoes? (contact dermatitis)
- Do you have a history of eczema? (inflammatory)
- Are there blisters? (dyshidrotic eczema or fungus)
If unsure, start with gentle care and monitor for improvement.
Step 2: Basic Home Care for All Types
These steps help most mild foot rashes:
- Wash feet daily with mild soap
- Pat dry completely (especially between toes)
- Avoid tight shoes
- Wear breathable cotton socks
- Change socks daily
- Let feet air out at home
Step 3: Targeted Treatments
For Fungal Foot Rash
Use over-the-counter antifungal creams like:
- Clotrimazole
- Miconazole
- Terbinafine
Apply twice daily for 2–4 weeks, even if symptoms improve early.
For Allergic Rash
- Stop using the suspected product
- Use a mild hydrocortisone cream (short-term)
- Take oral antihistamines if itching is severe
For Eczema
- Apply thick moisturizers daily
- Use steroid creams if prescribed
- Avoid hot water
For Bacterial Infection
See a doctor. You may need oral antibiotics.
How do you get rid of a foot rash fast?
To treat a foot rash quickly, keep the area clean and dry, use antifungal cream for fungal infections, apply hydrocortisone for allergic reactions, and avoid tight shoes. If symptoms worsen or don’t improve in one week, consult a doctor.
Natural Remedies
These may help mild cases:
- Coconut oil (moisturizing, mild antifungal)
- Aloe vera (soothing)
- Tea tree oil (antifungal dilute before use)
- Oatmeal soaks for itching
Note: Natural remedies support healing but don’t replace medical treatment for infections.
Prevention Strategies
Prevention is easier than treatment.
Daily Habits
- Dry feet thoroughly after bathing
- Change socks if sweaty
- Use antifungal powder if prone to fungus
- Wear breathable shoes
- Rotate shoes daily
- Avoid walking barefoot in public showers
For Sensitive Skin
- Choose fragrance-free products
- Test new shoes gradually
- Use hypoallergenic detergents
Common Mistakes People Make
Avoid these:
- Ignoring early symptoms
- Sharing shoes or socks
- Stopping antifungal cream too soon
- Scratching aggressively
- Using strong steroid creams without diagnosis
- Wearing damp shoes
These mistakes can worsen the rash or cause reinfection.
When to See a Doctor
Seek medical help if:
- Rash lasts more than 1–2 weeks
- It spreads rapidly
- You see pus or swelling
- You have diabetes
- There is severe pain
- You develop fever
- Over-the-counter treatment fails
People with diabetes should never ignore foot problems. Even small rashes can become serious.
Foot Rash in Children
Children often develop rashes from:
- Sweaty school shoes
- Allergic reactions
- Eczema
- Hand-foot-and-mouth disease (if accompanied by mouth sores and fever)
Always consult a pediatrician if a child has fever or widespread rash.
Foot Rash vs Other Conditions
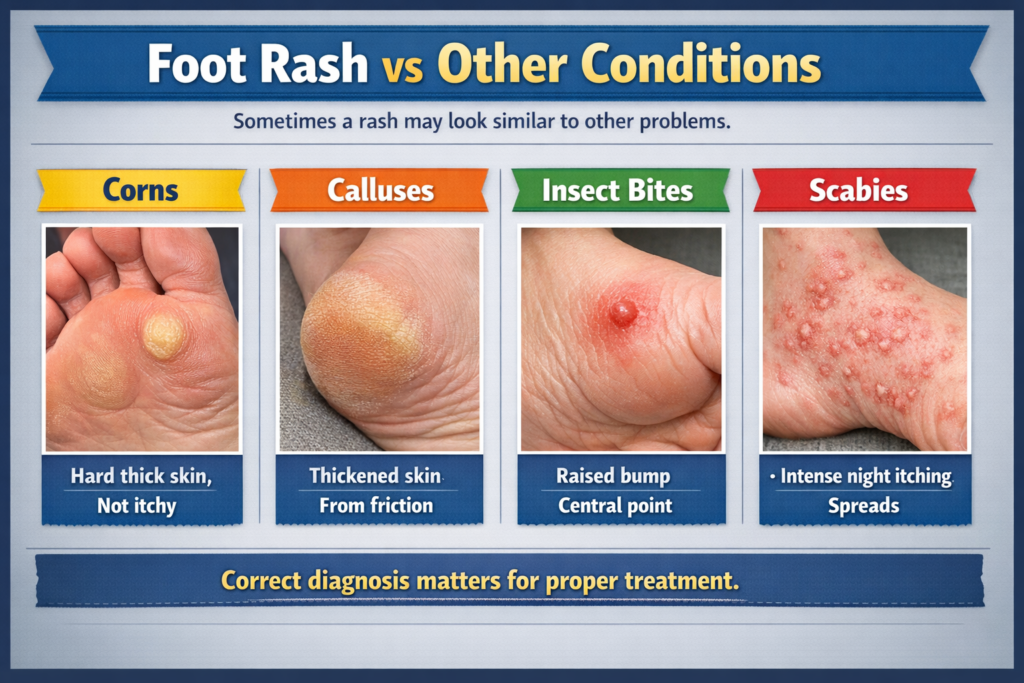
Sometimes a rash may look similar to other problems.
| Condition | Key Difference |
| Corns | Hard thick skin, not itchy |
| Calluses | Thickened skin from friction |
| Insect bites | Raised bump with central point |
| Scabies | Intense night itching, spreads |
Correct diagnosis matters for proper treatment.
Frequently Asked Questions (FAQs)
1. What is the most common cause of foot rash?
The most common cause is athlete’s foot, a fungal infection that thrives in warm, moist environments like sweaty shoes.
2. Is a foot rash contagious?
Fungal foot rashes are contagious and can spread through shared floors, shoes, or towels. Eczema and allergic rashes are not contagious.
3. How long does a foot rash take to heal?
Mild rashes may improve within a few days. Fungal infections often take 2–4 weeks of consistent treatment.
4. Can stress cause a foot rash?
Yes. Stress can trigger eczema and dyshidrotic eczema, leading to itchy blisters or dry patches on the feet.
5. Should I pop blisters from a foot rash?
No. Popping blisters increases the risk of infection. Keep them clean and covered.
6. Why does my foot rash keep coming back?
Recurring rashes often happen due to incomplete antifungal treatment, sweaty shoes, or untreated underlying skin conditions.
7. Can diabetes cause foot rashes?
People with diabetes are more prone to infections and slow healing, which can increase the risk of persistent foot rashes.
Final Thoughts
A foot rash may seem small, but it can become uncomfortable and even serious if ignored. The key is early identification, proper hygiene, and targeted treatment. Most rashes improve quickly when treated correctly.
If symptoms don’t improve, spread, or become painful, seek professional medical care. Healthy feet start with simple daily habits to keep them clean, dry, and protected.
Taking action early makes all the difference.